Irritable bowel syndrome (IBS) is a severe gastrointestinal condition characterized by symptoms such as pain, bloating, diarrhea, and constipation. Finding effective management strategies is crucial for individuals living with IBS. Recent research has highlighted the importance of glucagon-like peptide-1 (GLP-1) receptors in the central nervous system and peripheral tissues, which affect gut motility and may play a role in IBS symptoms.
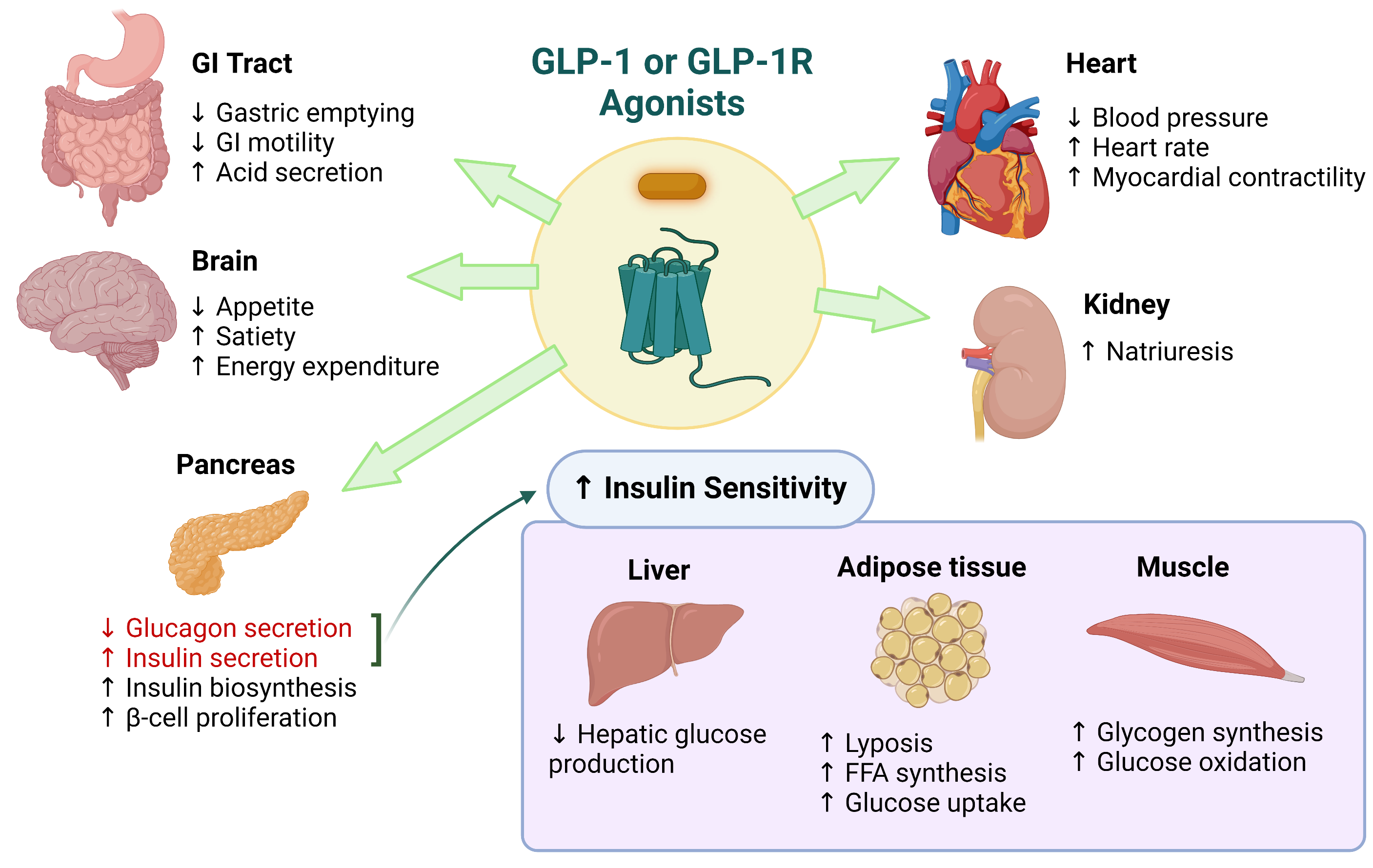
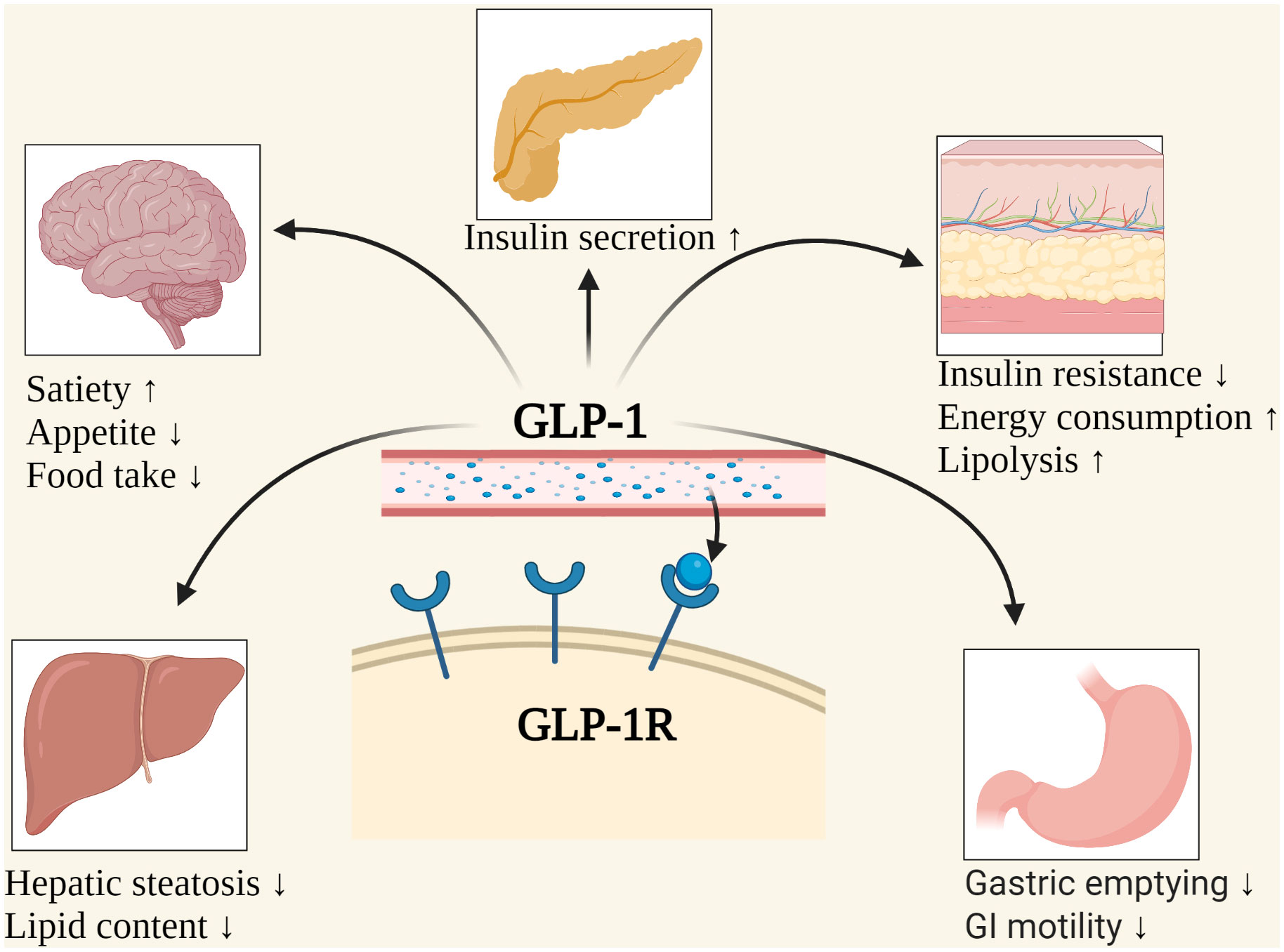
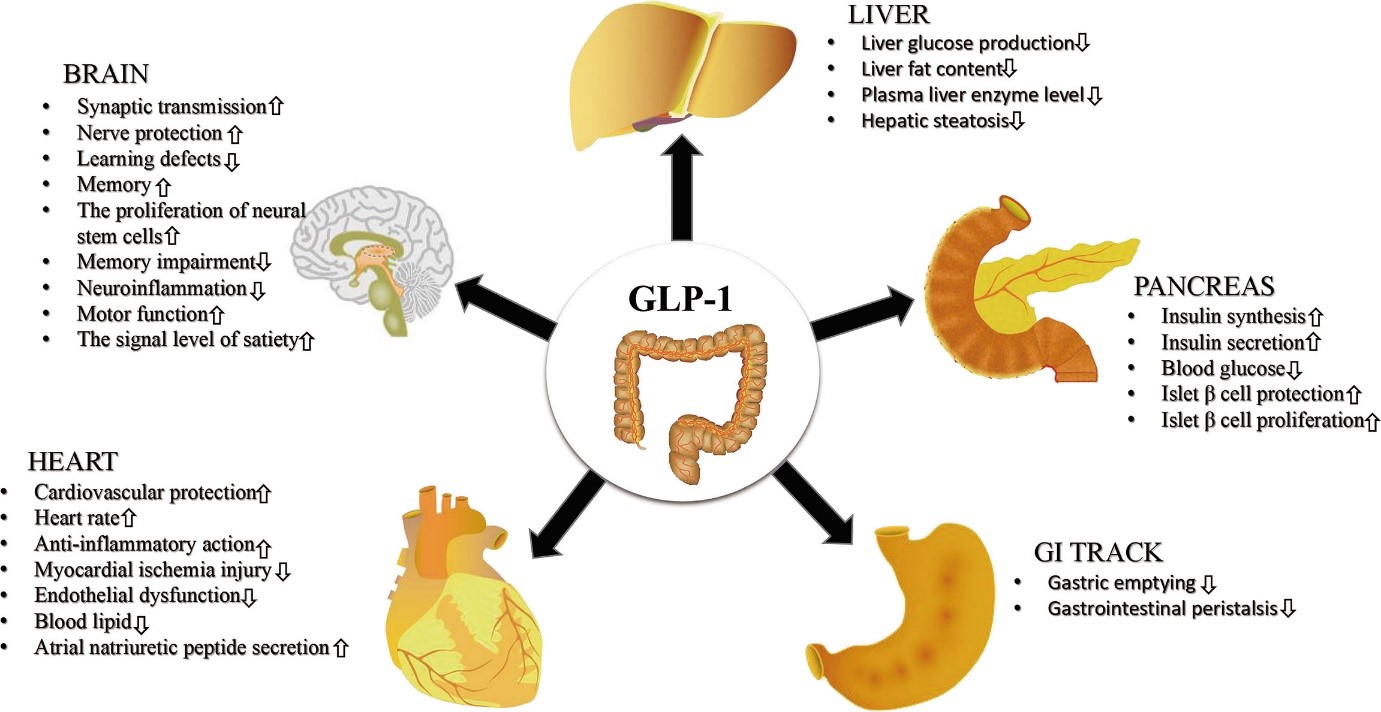
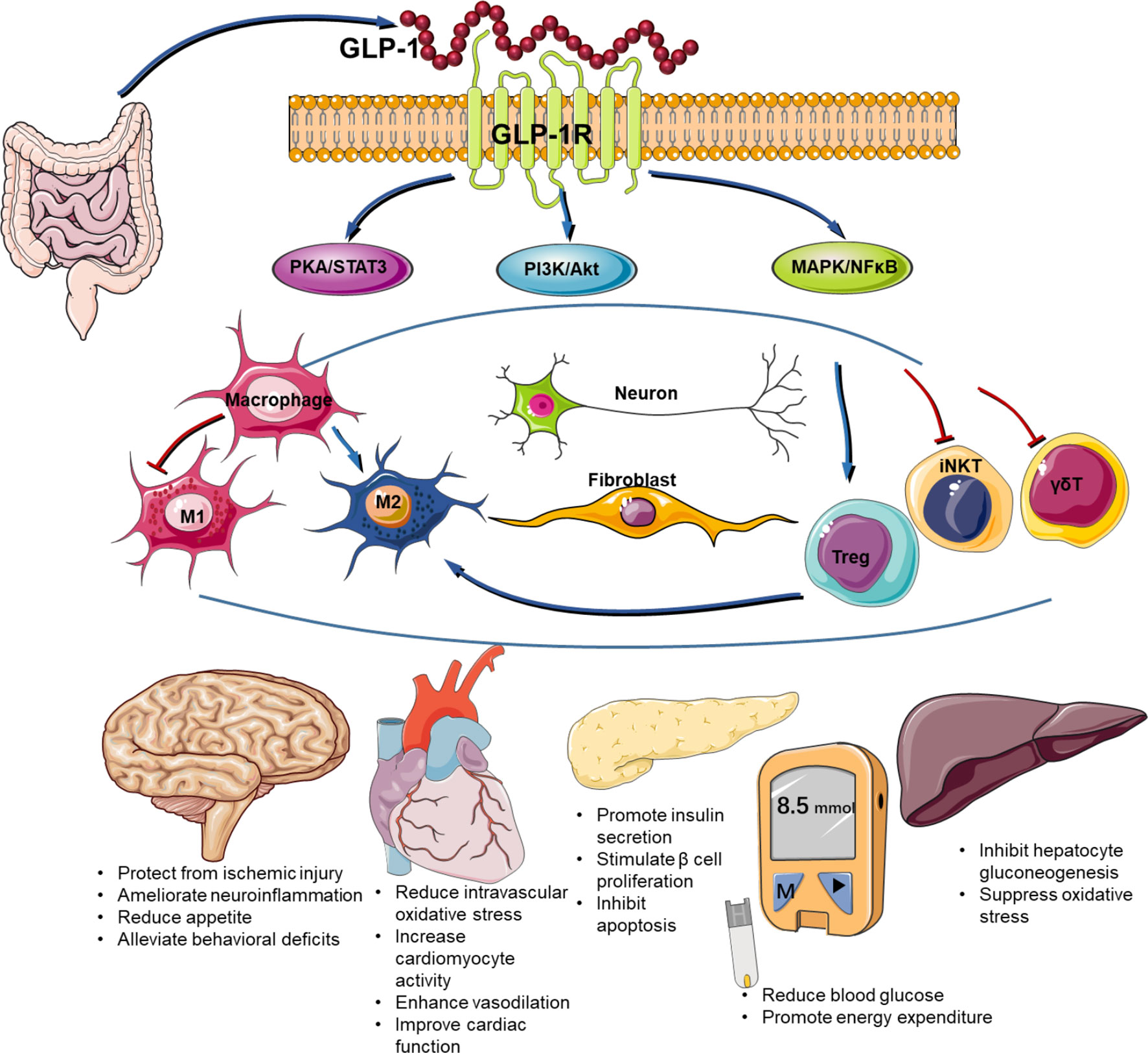
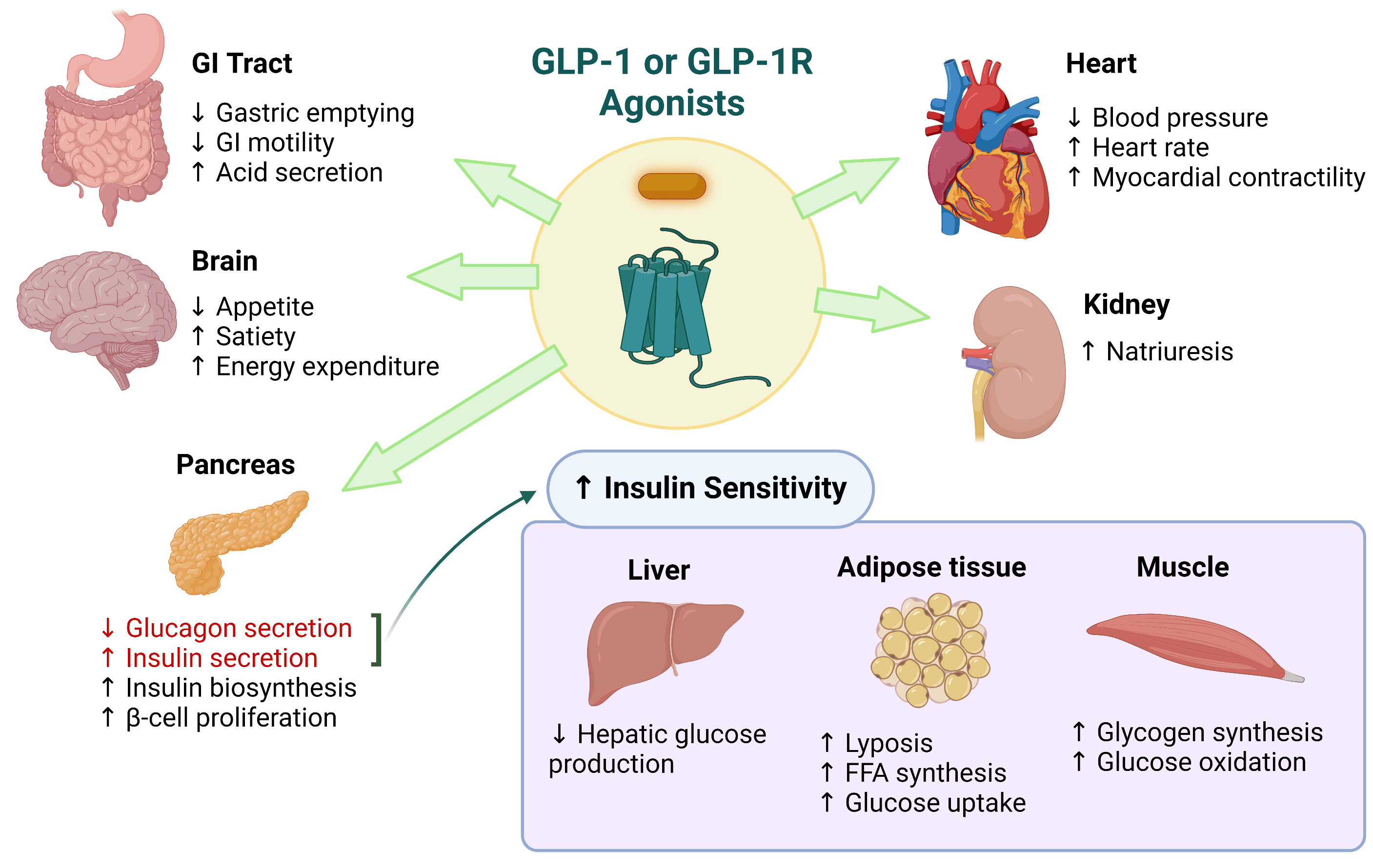
GLP-1 is a hormone that helps regulate blood sugar levels, appetite, and digestion. In individuals with IBS, GLP-1 signaling may be compromised, leading to altered gut function and symptom development. A growing body of evidence suggests that GLP-1 agonists, such as semaglutide (Ozempic, Wegovy), can alleviate IBS symptoms, but the underlying mechanisms remain poorly understood.
- GLP-1 receptors are expressed in the central nervous system and peripheral tissues, influencing gut motility and hormone signaling.
- Studies have shown that a low FODMAP diet may increase plasma GLP-1 levels in individuals with IBS, suggesting a potential link between dietary interventions and GLP-1 regulation.
- GLP-1 agonists have been shown to affect IBS symptoms, but more research is needed to fully understand the relationship between GLP-1 and IBS.
Mindful Eating for IBS: A Key Component of Management

Mindful eating is an essential component of managing IBS symptoms. By paying attention to hunger and fullness cues, recognizing emotional triggers, and developing a more structured eating plan, individuals with IBS can reduce reactive eating patterns and alleviate symptoms. Incorporating mindful eating practices into daily routines can also enhance gut health and support overall well-being.