Unlock the Power of GLP-1 and Insulin Sensitivity
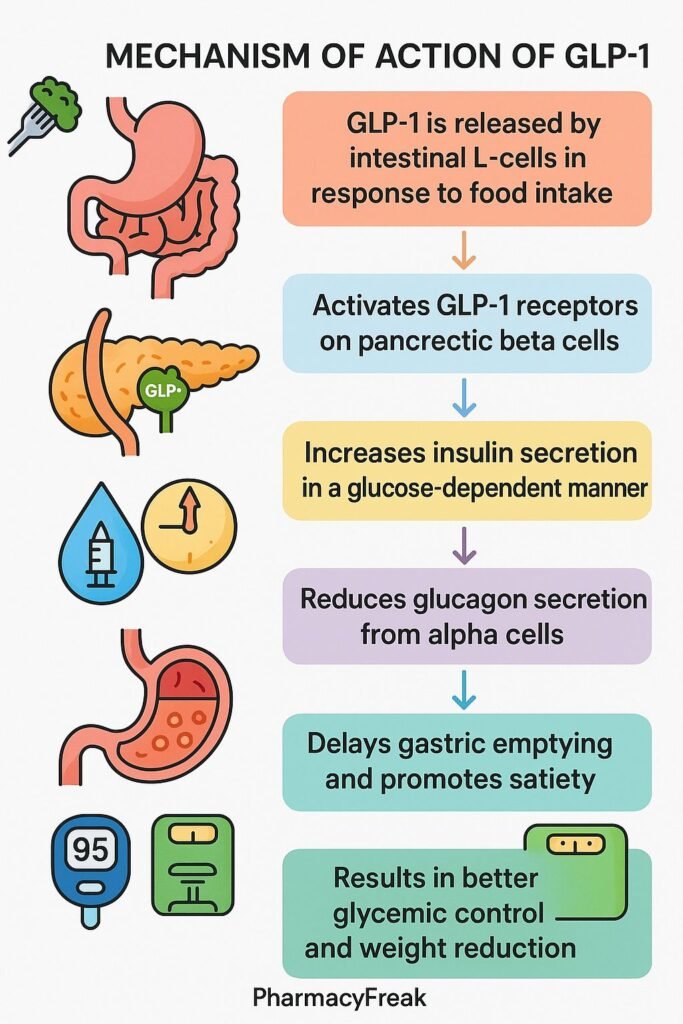
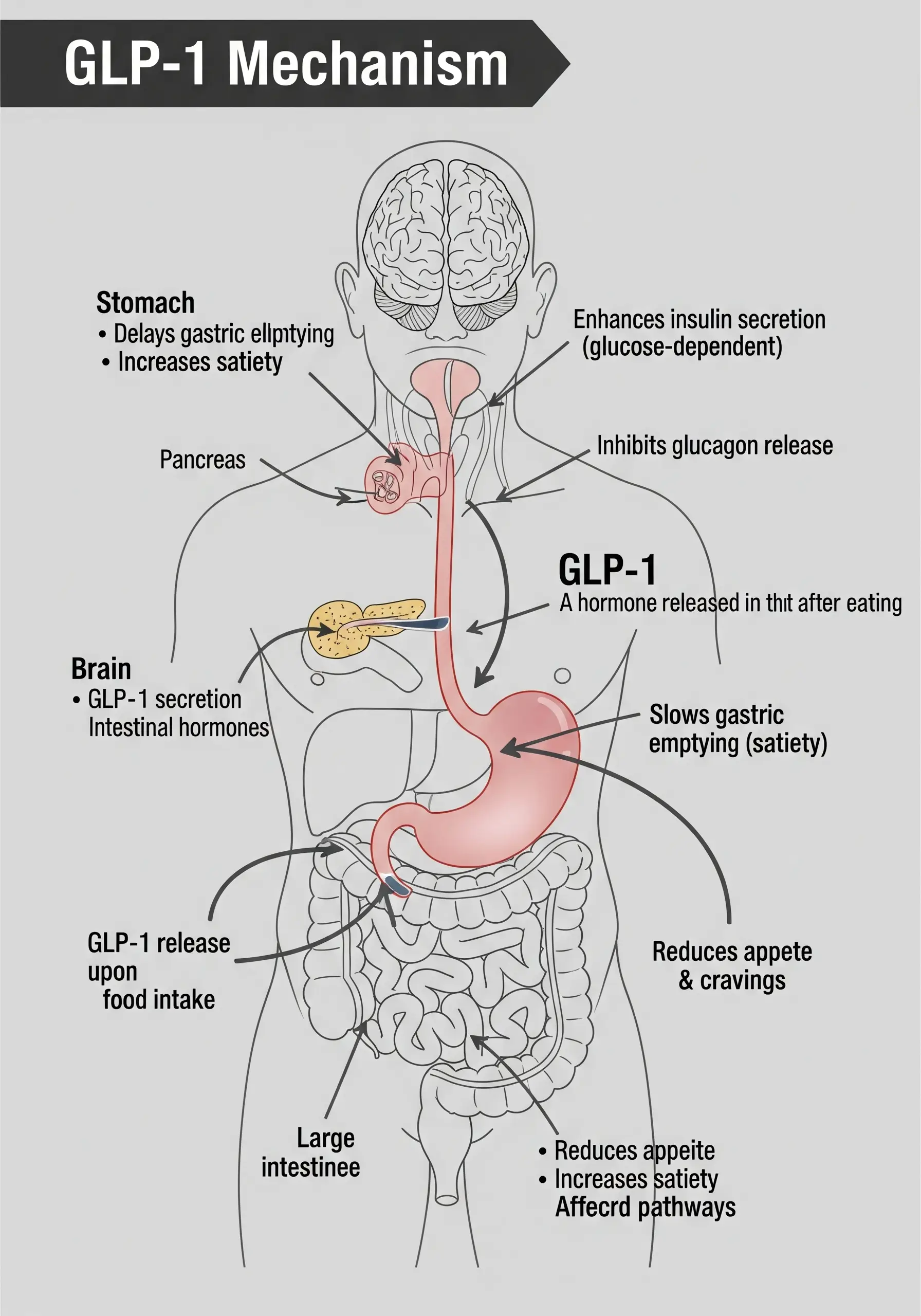
Glucagon-like peptide-1 (GLP-1) agonists have revolutionized the treatment of type 2 diabetes and associated metabolic disorders. These medications improve glycemic control by increasing insulin secretion, enhancing glucose uptake, and supporting healthy blood vessel function. However, despite their impressive weight loss promoting effect, GLP-1 receptor agonists do not normalize insulin sensitivity in individuals with type 2 diabetes. This article delves into the intricacies of GLP-1 and insulin sensitivity, exploring the complex relationships between these two critical components of glucose metabolism.
Understanding Insulin Sensitivity
Insulin sensitivity refers to the body's ability to effectively use insulin, a hormone produced by the pancreas that regulates blood sugar levels. When the body's cells respond well to insulin, glucose is absorbed, and blood sugar levels are maintained within a normal range. Conversely, insulin resistance occurs when the body's cells become less responsive to insulin, leading to elevated blood glucose levels and contributing to the development of type 2 diabetes.

How GLP-1 Impacts Insulin Sensitivity
GLP-1, a hormone released after meals, plays a vital role in regulating insulin sensitivity. By enhancing insulin secretion, improving glucose uptake, and reducing inflammation, GLP-1 agonists help optimize insulin sensitivity. Moreover, studies have shown that GLP-1 can improve insulin sensitivity in the brain, which is essential for proper cognitive function.